Patient presentation
The patient, an international referral, presented with primary developmental breast asymmetry — no prior breast surgery. The clinical findings on examination were:
- Right breast approximately 50–60% larger than the left
- Right breast ptotic — nipple-areola complex (NAC) sitting below the level of the inframammary fold (Regnault grade II–III ptosis)
- Left breast smaller, with NAC at appropriate level relative to its inframammary fold
- No skin envelope abnormalities, no underlying chest wall asymmetry, no glandular masses
Her goal was symmetry — both in size and shape — with a final result that would let her wear standard bras and clothing without specialised fitting. She was prepared for the asymmetric scar burden that achieving symmetry would require.
The symmetry problem — why this isn't simple bilateral augmentation
Naive intuition suggests "just use a bigger implant on the smaller side." This does not work for this case for two reasons:
- The right breast is too large already. Implant volume only adds; it cannot reduce. Augmenting the left to match the right would leave both breasts excessively large for the patient's frame, and the right would still be ptotic.
- The right breast is ptotic. No volume change on either side fixes nipple position. A breast lift (mastopexy) is the only way to elevate the NAC. A larger implant on a ptotic breast typically makes ptosis worse — the implant slides down with the existing soft-tissue envelope.
The clinical insight is that achieving symmetry requires different operations on each side, calibrated so the post-operative breasts match in size, shape, and NAC position. This is the planning that distinguishes a complex asymmetric case from a routine bilateral augmentation.
Why different operations on each side
Left side — augmentation only
The left breast had appropriate skin envelope, normal NAC position, and adequate soft-tissue cover. Adding implant volume produced the desired enlargement without disturbing what already worked. A simple inframammary fold incision was used, with subfascial implant placement.
Right side — superior-pedicle inverted-T reduction-augmentation mastopexy
The right breast required three things at once:
- Reduction — to remove excess glandular and adipose tissue, bringing volume down toward what the left side would become with augmentation
- Mastopexy (lift) — to elevate the NAC to its anatomically correct position above the inframammary fold
- Augmentation — to add the same 375 cc implant used on the left, ensuring the final volume composition matches
Doing all three in a single operation is technically demanding because the blood supply to the NAC must be preserved while large amounts of tissue are rearranged. The pedicle technique (next section) is what makes this safe.
Why the same implant size on both sides
It would be easy to assume that the smaller left breast needs a larger implant than the right (which is being reduced). In fact the opposite is more often true — using the same implant size on both sides simplifies long-term symmetry.
The reasoning: if the right breast is reduced down to the volume of the left and then both receive the same 375 cc implant, the final breast volumes are identical and the soft-tissue cover behaves similarly on each side. Future life events — weight changes, pregnancy, aging — will affect both sides equivalently. Asymmetric implant volumes would be likely to produce visible asymmetry over time as the soft tissue evolves differently on each side.
The reduction target on the right is therefore set with the implant volume in mind: reduce to a glandular volume on the right that, with a 375 cc implant added, matches the left's glandular volume plus the same 375 cc.
Why a superior pedicle
In a reduction or mastopexy, the NAC must remain attached to a vascular pedicle — a column of tissue that carries arterial supply and venous drainage to the nipple. Several pedicle designs exist (superior, inferior, medial, superomedial, inferolateral), each with different geometry and indications.
The superior pedicle was chosen here for three reasons:
- Reliable vascularity for moderate elevation. The superior pedicle reliably carries blood supply when the NAC needs to be elevated by a moderate distance — appropriate for this patient's grade II–III ptosis.
- Compatibility with concurrent augmentation. The superior pedicle works well alongside an implant placed in the subglandular or subfascial plane — the pedicle and the implant occupy different spaces and do not compete for tissue.
- Long-term shape stability. Superior-pedicle techniques tend to maintain upper-pole fullness over time, which is desirable when an implant is also providing structure.
For very long pedicle distances or larger reductions, an alternative (such as inferior or medial pedicle) might be safer; for this case, the geometry favoured superior.
Why an inverted-T scar pattern
Mastopexy and reduction techniques are categorised partly by their scar pattern. The main options are:
- Periareolar (donut) — scar around the NAC only. Limited correction; suitable only for minimal ptosis.
- Vertical (lollipop) — scar around NAC plus a vertical limb to the inframammary fold. Good for moderate ptosis; smaller scar burden than inverted-T.
- Inverted-T (anchor / Wise pattern) — scar around NAC, vertical limb, and a horizontal inframammary limb. Largest scar but allows the most correction.
The inverted-T pattern was selected here because the volume of tissue requiring redistribution was significant. Vertical-only techniques are excellent for moderate cases, but in cases requiring substantial reduction and mastopexy and augmentation, the inverted-T provides the necessary access and skin redraping precision. The horizontal inframammary scar fades well and is hidden by clothing and bras.
This patient was counselled in detail about the scar trade-off — accepting more scar to achieve precise symmetry was her informed choice.
Surgical plan
- Anaesthesia: General, board-certified anaesthesiologist, JCI-accredited hospital
- Operative time: Approximately 4 hours (asymmetric work; right side longer than left)
- Pre-op marking: Performed with patient standing, prior to anaesthesia. Mid-clavicular line, breast meridian, inframammary fold position, planned NAC position, and inverted-T scar pattern marked on the right.
- Left side: Inframammary fold incision; subfascial pocket dissection; 375 cc round high-projection implant placement; layered closure.
- Right side: Inverted-T (Wise pattern) skin incision; superior-pedicle de-epithelialisation; reduction of inferior-pole tissue to the planned volume; subfascial pocket dissection; 375 cc round high-projection implant placement; NAC repositioning on the superior pedicle; vertical and horizontal scar closure with layered absorbable sutures.
- Triple-antibiotic irrigation of both implant pockets prior to placement.
- Drains: Right side only (because of the larger dissection), removed at 3–5 days.
- Hospital stay: One overnight.
Photos — pre-op and Day 5 post-op
Note on Day 5 photographs. The post-operative images shown below are taken five days after surgery. At this stage: the implants sit higher than their final position (drop over 6–8 weeks), the right side scars are pink and firm, swelling on the right (the more extensively operated side) is greater than on the left and resolves at a slightly slower pace. The right breast may appear slightly different from the left at Day 5 — this asymmetric early swelling is expected and resolves by 6–8 weeks. Final symmetry is judged at 6–12 months once both sides have settled.
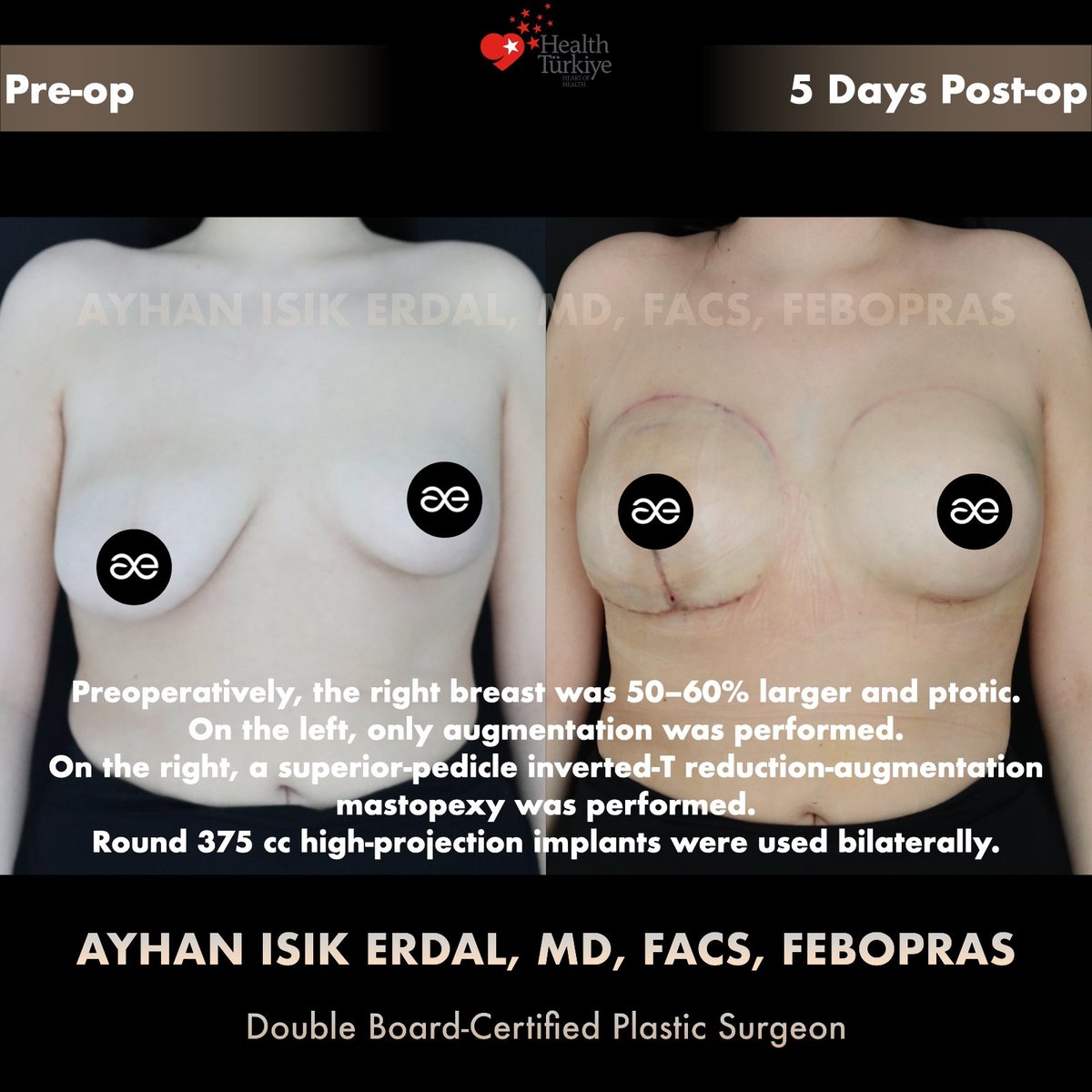
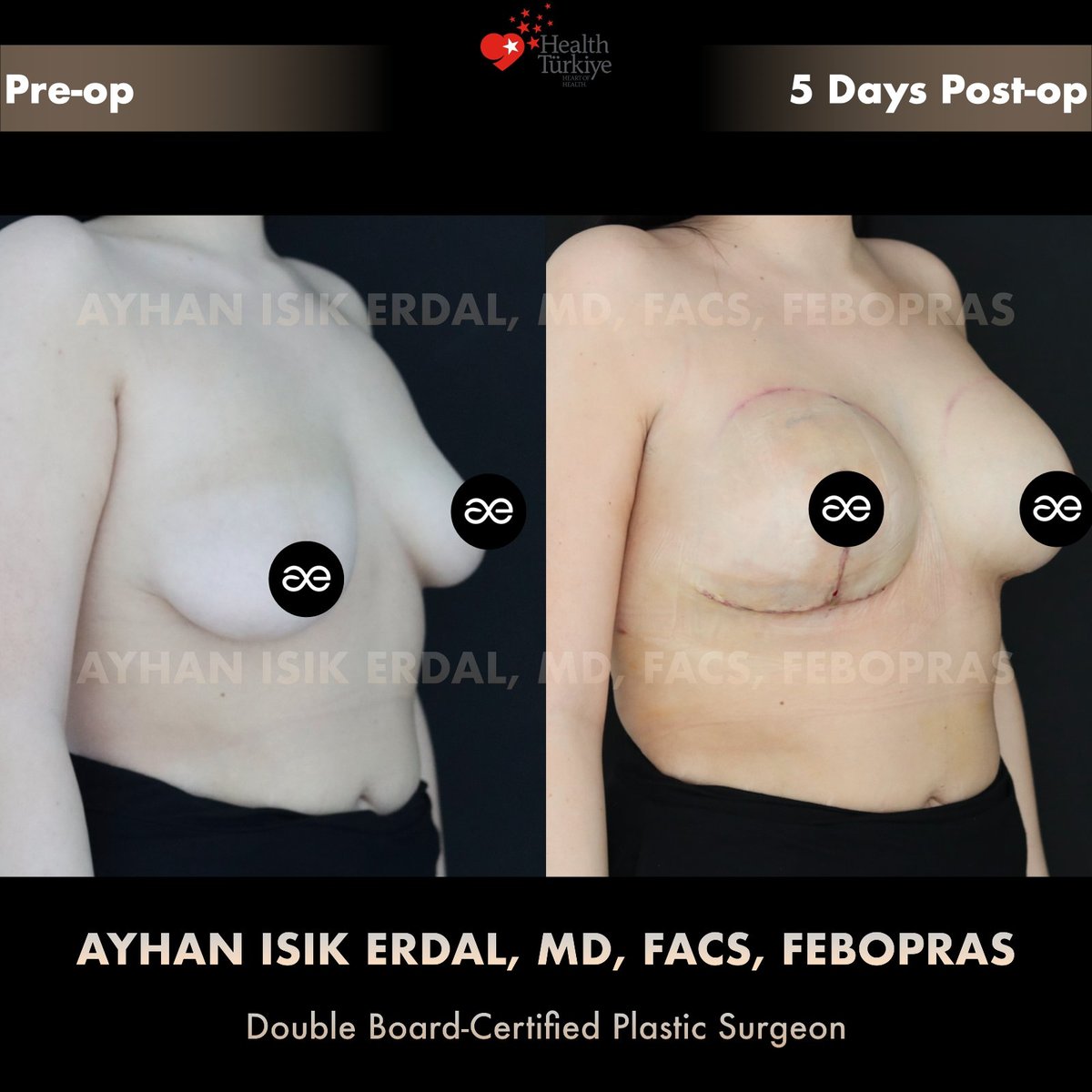
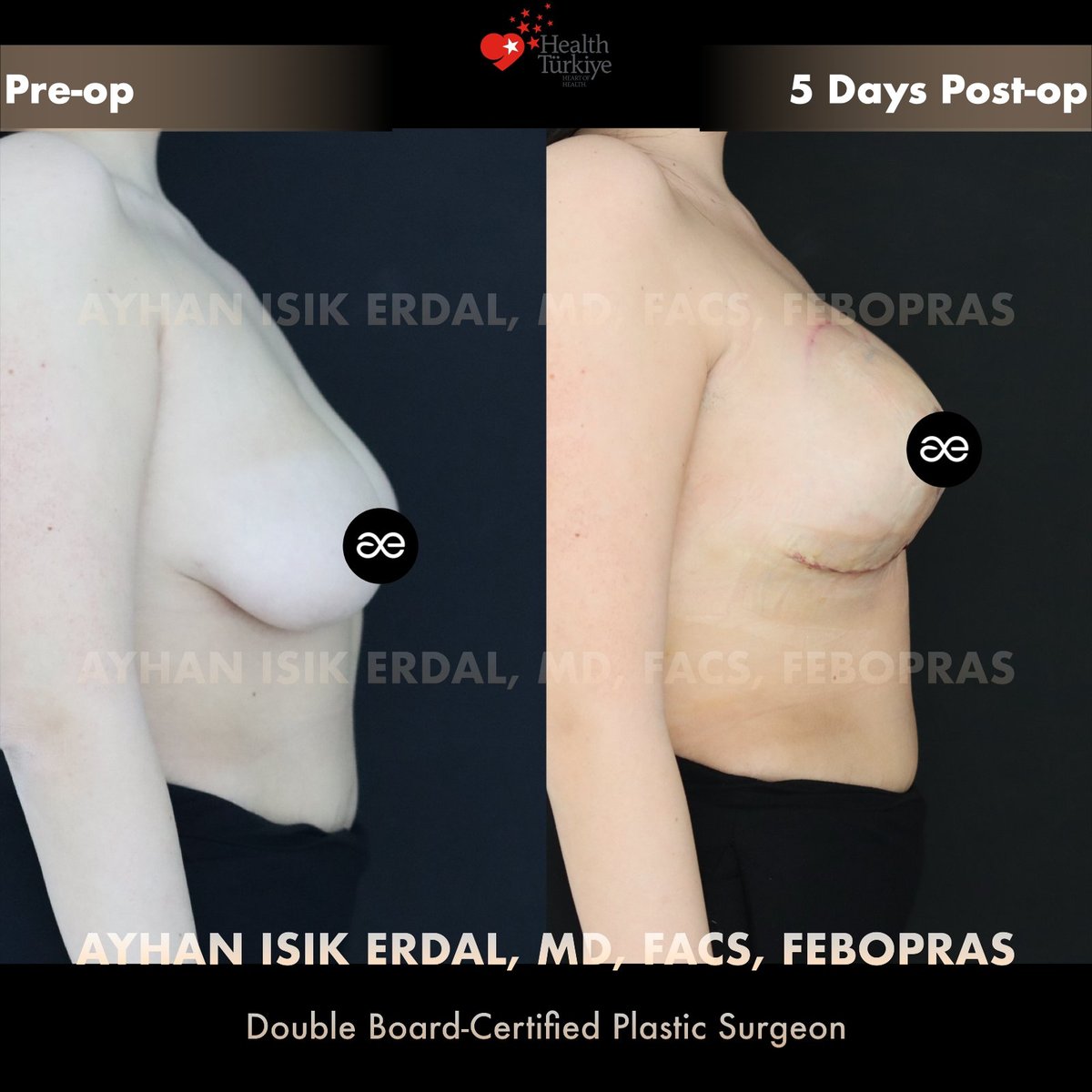
Early recovery — what you see at Day 5
- Asymmetric swelling. The right side received much more dissection than the left and is correspondingly more swollen at Day 5. This evens out by week 4–6.
- Visible inverted-T scars on the right. Periareolar, vertical, and horizontal inframammary scar lines are pink and firm. They will fade over 6–12 months.
- Single inframammary scar on the left. Only the implant insertion incision; smaller scar burden.
- NAC viability check. The right NAC is monitored carefully in the first 72 hours for any sign of vascular compromise. In this case, the NAC remained well-perfused throughout.
- Implants sitting high. Both implants are in fresh pockets and have not yet settled. Drop into final position takes 6–8 weeks.
- Activity restriction. No upper-body lifting for 4 weeks; no resistance training for 6–8 weeks.
Expected trajectory from Day 5 to final outcome
- Week 1 (Day 5 photo): Implants high, right side swollen more than left, fresh scars pink.
- Weeks 2–4: Implants begin dropping. Swelling difference between sides reduces. Scar tape and silicone gel begin.
- Weeks 4–8: Implants drop into final position. Asymmetric early swelling resolves; the two sides start to match in volume and shape.
- Months 3–6: Final volume and shape match. NAC position stable on the right. Scars start to fade from pink toward skin tone.
- Months 6–12: Final aesthetic outcome. Inverted-T scars mature into fine lines; periareolar scar typically the most visible but still acceptable; vertical limb fades; horizontal inframammary limb hidden by undergarments.
- Years 1+: Long-term symmetry preserved by using the same implant volume on both sides — the soft tissue ages equivalently on each side.
What this case demonstrates
- Symmetry is achieved by matching final volume and shape — not by matching the operation performed on each side. Different problems require different operations even when the goal is identical.
- Using the same implant size on both sides simplifies long-term symmetry and is the right choice in most asymmetric reduction-augmentation cases. Varying implant size between sides is a short-term fix that becomes a long-term symmetry problem.
- Pedicle and scar pattern are independent decisions. Pedicle is chosen for vascular safety (anatomy + elevation distance + concurrent operations); scar pattern is chosen for the amount of skin redraping needed. The two often go together but are distinct technical choices.
- Patients accepting a complex asymmetric correction should understand the asymmetric scar burden — one side has a single scar, the other has three. This is part of how symmetry is achieved and is worth the trade-off when symmetry is the priority.
- Day 5 photos honestly show asymmetric early swelling. Patients prepared for the trajectory ("the side that had more surgery looks more swollen at first, and that evens out") are not anxious about the early asymmetry; patients expecting day-1 symmetry are.
Have asymmetric or complex anatomy?
If your case involves significant asymmetry, anatomical anomaly, or requires combined reduction + lift + augmentation, send your photos and history for a written assessment of the planning that would apply.
Free WhatsApp Consultation