Patient presentation
The patient, an international referral, presented several years after a primary submuscular breast augmentation that had healed without complication. Her original 275 cc implants were comfortable, well-positioned, and free of capsular contracture. She had no medical reason to revise.
What she wanted was specific:
- A modest volume increase — slightly fuller, not dramatically larger
- Softer transition between the implants and her sternum (the cleavage edge)
- To keep the same plane and incision, since both had served her well
- An updated implant rather than continuing with implants approaching the 10-year mark
This is a common revision profile: not a complication, not a regret — a refinement. The clinical task is to deliver the requested change without disturbing what already worked.
Why hybrid (implant + fat) instead of a larger implant alone
Patients with relatively thin medial soft-tissue cover sometimes show a visible "ledge" where the implant ends and the chest wall begins — particularly visible at the upper-medial pole when wearing low necklines. Going to a larger implant alone does not soften this transition; it often makes it more prominent because the implant edge becomes more palpable in thin tissue.
The technical solution is composite (or "hybrid") augmentation: implant volume for projection and structure, plus a small amount of autologous fat layered into the medial soft-tissue zone to feather the edge. The implant gives the bulk; the fat blends the boundary so the cleavage transition reads as continuous tissue rather than as the edge of a pocket.
For this patient — modest volume increase, thin medial cover, naturalness as the explicit goal — the hybrid approach was clinically appropriate and produced exactly the result she described in consultation.
Why the same plane (no plane change)
A common revision question is whether to change the implant plane (subglandular ↔ subfascial ↔ submuscular). Plane change adds operative complexity and recovery time, so it should be reserved for cases where the existing plane caused problems.
This patient's submuscular plane had served her well: no rippling, no animation deformity bothering her, no recurrent contracture, and adequate soft-tissue cover for the new (slightly larger) implant. There was no clinical reason to change something that was working.
Same-plane revision uses the existing pocket — modified slightly for the new implant's footprint — and avoids the additional dissection and recovery of a plane change. The original IMF incision is reopened, the existing implant removed, the pocket assessed and adjusted, the new implant placed.
Why a full capsulectomy on a healthy capsule
The existing capsule was clinically soft (Baker I) — there was no contracture indication for capsulectomy. Despite this, full capsulectomy was performed for three reasons:
- Pocket optimisation. A full capsulectomy creates a fresh tissue plane that conforms precisely to the new larger implant. The old capsule was sized for a 275 cc implant; leaving it in place would have constrained how the 400 cc implant settled.
- Surface change opportunity. Since the implants are being exchanged anyway, this is the natural moment to switch from any older textured surface to a smooth-surface implant — current evidence supports smooth surfaces for lower long-term BIA-ALCL risk. A fresh pocket without the old textured-implant capsule reduces residual contamination.
- Long-term stability. Capsulectomy in an older but healthy capsule slightly reduces the risk of late capsular contracture in the new pocket, particularly when combined with triple-antibiotic irrigation and a no-touch insertion technique.
Capsulectomy in a soft, healthy capsule is a deliberate choice rather than a default — it is offered when the technical advantages outweigh the slightly extended operative time and recovery.
Surgical plan
- Anaesthesia: General, board-certified anaesthesiologist, JCI-accredited hospital
- Operative time: Approximately 3 hours (capsulectomy + exchange + fat harvest + grafting)
- Incision: Existing inframammary fold (IMF) scar reopened — no new scars
- Implant removal and full capsulectomy
- Pocket adjustment for the new implant footprint
- Triple-antibiotic irrigation (bacitracin / cefazolin / gentamicin) of the fresh pocket
- New implant placement — 400 cc smooth-surface, submuscular, with no-touch insertion sleeve
- Donor site fat harvest from abdomen / flanks at low negative pressure
- Fat processing to isolate viable adipose fraction
- Cleavage fat grafting: approximately 50 cc per side (~100 cc total) layered into medial subcutaneous tissue with retrograde injection technique
- Layered closure of the IMF incision
- Drains: brief drain placement; removed before discharge
- Hospital stay: one overnight
Photos — pre-op and Day 4 post-op
Note on Day 4 photographs. The post-operative images shown below were taken four days after surgery, before discharge. At this stage: the implants sit higher than their final position (they "drop" gradually over 6–8 weeks), post-injection oedema in the cleavage zone is at its peak, microporous tape protects the IMF incisions, and the scars are pink and firm. The aesthetic outcome at Day 4 is therefore not the final result. Final shape and scar maturation are judged at 6–12 months.
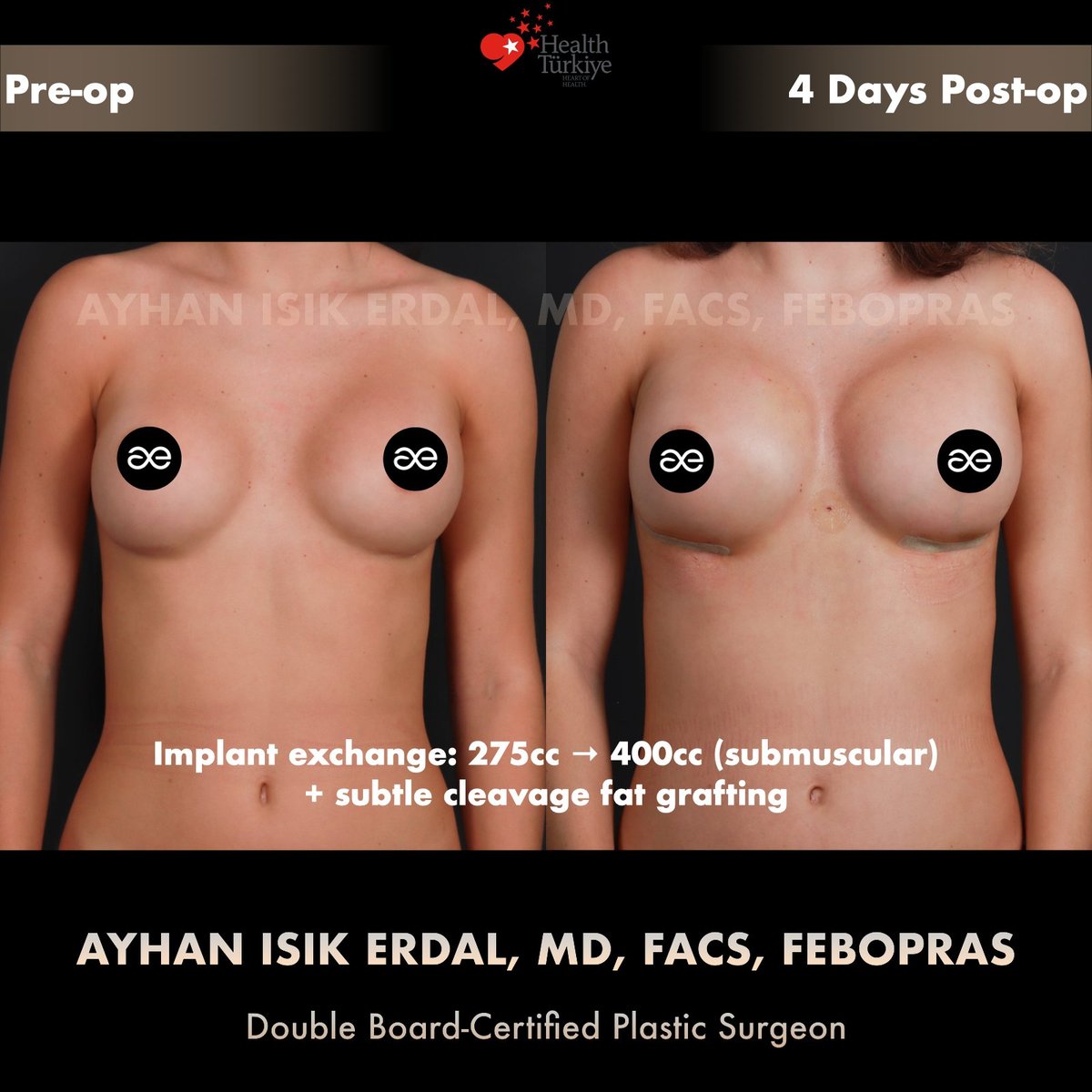
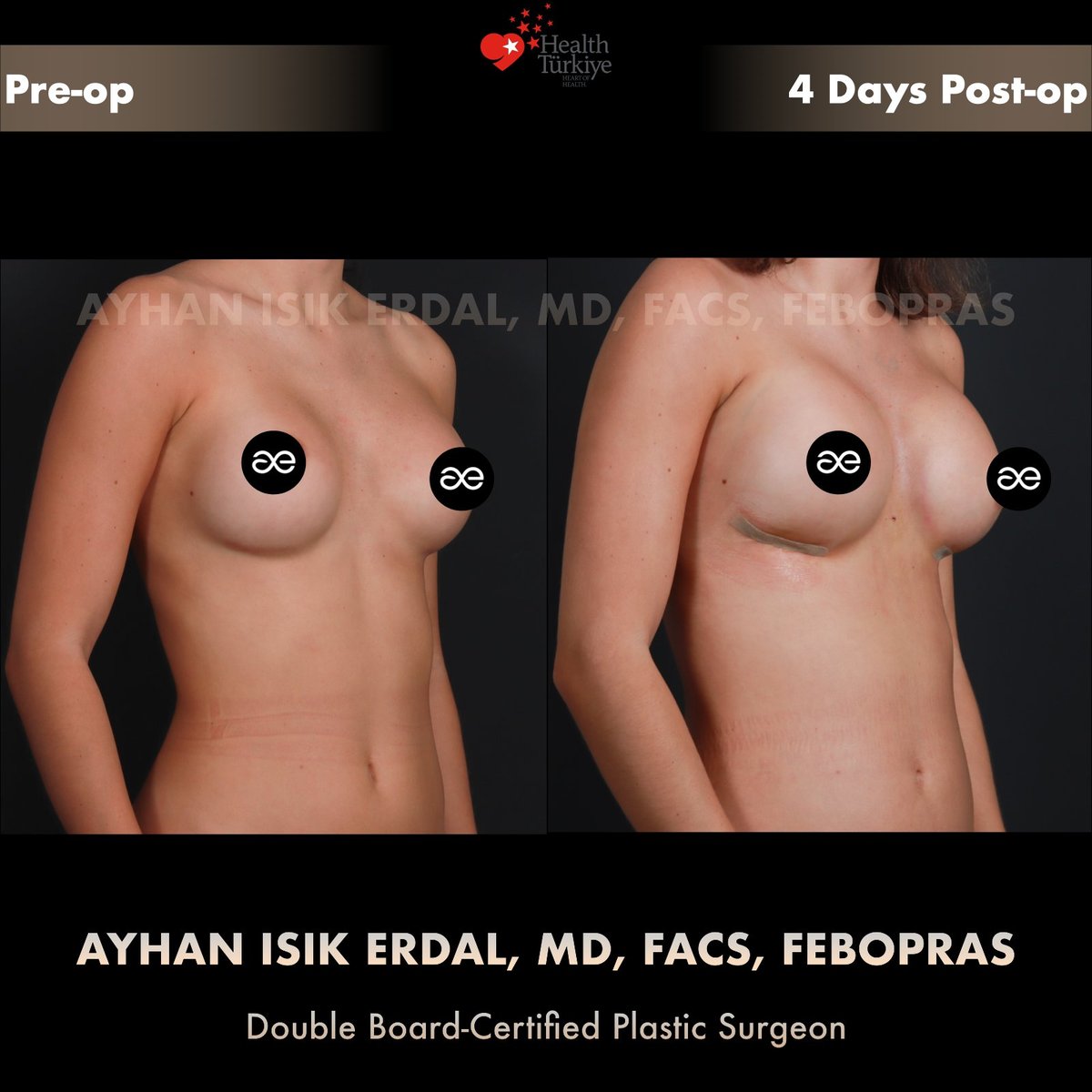
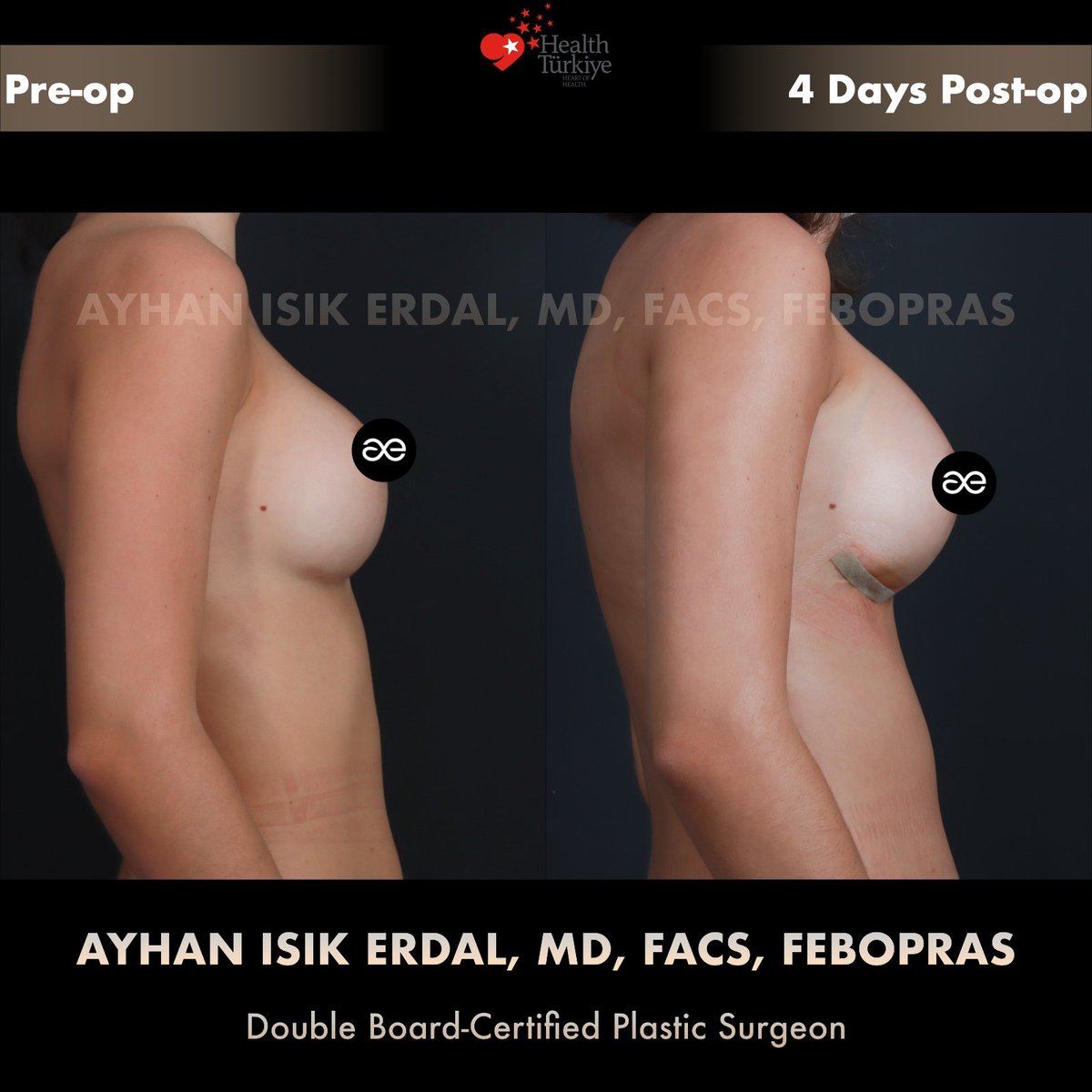
Technique notes
Capsulectomy with intact capsule
Full capsulectomy on a soft, intact capsule is technically more straightforward than capsulectomy on a contracted one — the tissue planes are clean, bleeding is controlled, and the capsule can usually be removed in one or two pieces. The dissection stays directly on the capsule wall to avoid violating surrounding muscle or fascia.
Pocket adjustment for the new implant
The fresh pocket is then sized to the 400 cc implant's footprint. For a 125 cc volume increase in the same plane, only modest pocket expansion is needed — typically a few millimetres laterally and inferiorly. Aggressive expansion is avoided because it predisposes to malposition.
Cleavage fat grafting placement
For the medial cleavage zone, fat is placed in the subcutaneous and superficial subfascial planes — never inside the implant pocket. The plane that needs filling is the soft-tissue cover over the medial implant edge, not the pocket itself.
Approximately 50 cc per side is delivered through small cannulas with retrograde injection on withdrawal, in many small parcels rather than single large boluses. The volume is deliberately conservative — cleavage fat grafting is for refinement, not bulk volume change. Larger cleavage fat volumes risk visible irregularity or fat necrosis in this thin tissue zone.
Early recovery — what you see at Day 4
- Implants sit high. The new pocket is freshly dissected, so the implants haven't yet settled to their final position. Patients sometimes worry their implants are "too high" at Day 4 — this is normal and resolves over 6–8 weeks as the muscle relaxes and the pocket softens.
- Cleavage swelling. The grafted cleavage zone is oedematous and may look fuller than the final result. Some of the apparent volume here is post-injection fluid, not fat — true fat volume is judged at 6 months.
- IMF scar dressings. Microporous tape supports the incision and is left in place for 1–2 weeks. The scar underneath will be pink and firm at this stage; full maturation takes 12 months.
- Donor site discomfort. Abdomen and flanks where fat was harvested are tender and bruised. Compression garment for 4–6 weeks at the donor site.
- Pain. Generally well-controlled with oral analgesics; comparable to primary submuscular augmentation. Most patients return to office work within 7–10 days.
Expected trajectory from Day 4 to final outcome
- Week 1 (Day 4 photo): Implants high, cleavage fat-graft zone swollen, scars taped.
- Weeks 2–4: Implants begin to drop. Cleavage swelling reduces noticeably. Scar tape removed; daily silicone gel begins.
- Weeks 4–8: Implants drop into final position. Upper-pole softens. Cleavage zone consistency settles as fat-graft oedema fully resolves.
- Months 3–6: Final implant position and shape. Fat resorption stabilises (typically 30–40% of grafted volume resorbs; the rest is permanent). Scars start fading from pink toward skin-tone.
- Months 6–12: Final aesthetic outcome. Cleavage transition smooth and natural. Scars mature to fine lines along the IMF.
What this case demonstrates
- Hybrid breast augmentation (implant + fat) addresses problems that neither modality solves alone — particularly the medial cleavage transition in patients with thin soft-tissue cover.
- Same-plane revision is the right choice when the existing plane has not caused problems. Plane change is added only when the existing plane is the clinical issue, not as a default.
- Full capsulectomy on a healthy capsule is a deliberate, justified choice — it allows pocket optimisation, surface change, and reduced future contracture risk. It is not the default but it has clear indications.
- Day 4 photographs honestly show what fresh post-operative tissue looks like — high implants, swollen fat-graft zone, taped scars. Patients prepared for this trajectory are not anxious about it; patients expecting "final-result" appearance immediately are. Realistic expectations are part of revision planning.
- Refinement-driven revision (no complication, just goal evolution) is a legitimate indication and one of the more rewarding case types to perform — the patient already knows what she wants and the clinical task is precise execution.
Considering an implant exchange with refinement?
If your existing breast augmentation is fine but you want a modest size change or refinement (cleavage softening, profile update, surface change), send your photos and implant card details for a written assessment.
Free WhatsApp Consultation