Patient presentation
The patient, an international referral, presented after a previous breast surgery that had been complicated by infection. The full operative history was incomplete — she had not retained operative records and could not specify exactly which procedure(s) had been performed before. What was clinically apparent on examination:
- Asymmetric volume between the two breasts
- Visible contour deformity, more pronounced on one side
- Skin envelope showing prior surgical changes (visible on close inspection)
- No active infection, no implants currently in place, soft tissue stable
Her stated goal was symmetry and modest restoration of volume. She did not want implants — and given the history of infection, she was relieved to learn that an implant-free correction was possible.
Why fat grafting, not implants
Several factors converged to make autologous fat transfer the right choice for this case rather than a revision augmentation with implants:
Patient preference
The patient explicitly did not want a prosthetic placed in tissue that had previously been infected. This is a reasonable concern — re-implantation in a previously infected pocket carries higher risk of recurrent infection or capsular contracture than implantation in virgin tissue.
Tissue history
Previously infected and operated tissue does not behave the same as virgin tissue. Scar tissue planes, altered vascularity, and variable soft-tissue cover all complicate implant-based revision. Fat transfer works with the existing tissue rather than against it — adding volume in a way that integrates with the patient's own anatomy.
Goal alignment
The volume increase needed was modest. The patient was not seeking dramatic enlargement; she wanted symmetry and the restoration of natural contour. Fat grafting is well-suited to this goal — high-volume implants would have been overkill, and lower-volume implants in damaged tissue would have produced visible rippling and palpable edges.
Donor site availability
The patient had adequate fat reserves at standard donor sites (abdomen, flanks) to harvest the volume needed without over-aggressive liposuction. Fat grafting is only viable when the donor site can supply sufficient volume — in patients with very low body fat, this is the limiting factor.
Surgical plan
- Anaesthesia: General anaesthesia, board-certified anaesthesiologist, JCI-accredited hospital
- Operative time: Approximately 3 hours
- Donor sites: Abdomen and flanks (also providing modest abdominal contouring as a secondary benefit)
- Harvest volume: Sufficient lipoaspirate to yield 400 cc of processed fat for injection
- Injection volume: 400 cc total, distributed across both breasts proportionally to address the asymmetry
- Hospital stay: One night for monitoring
- Drains: Donor site drainage management; no breast drains required
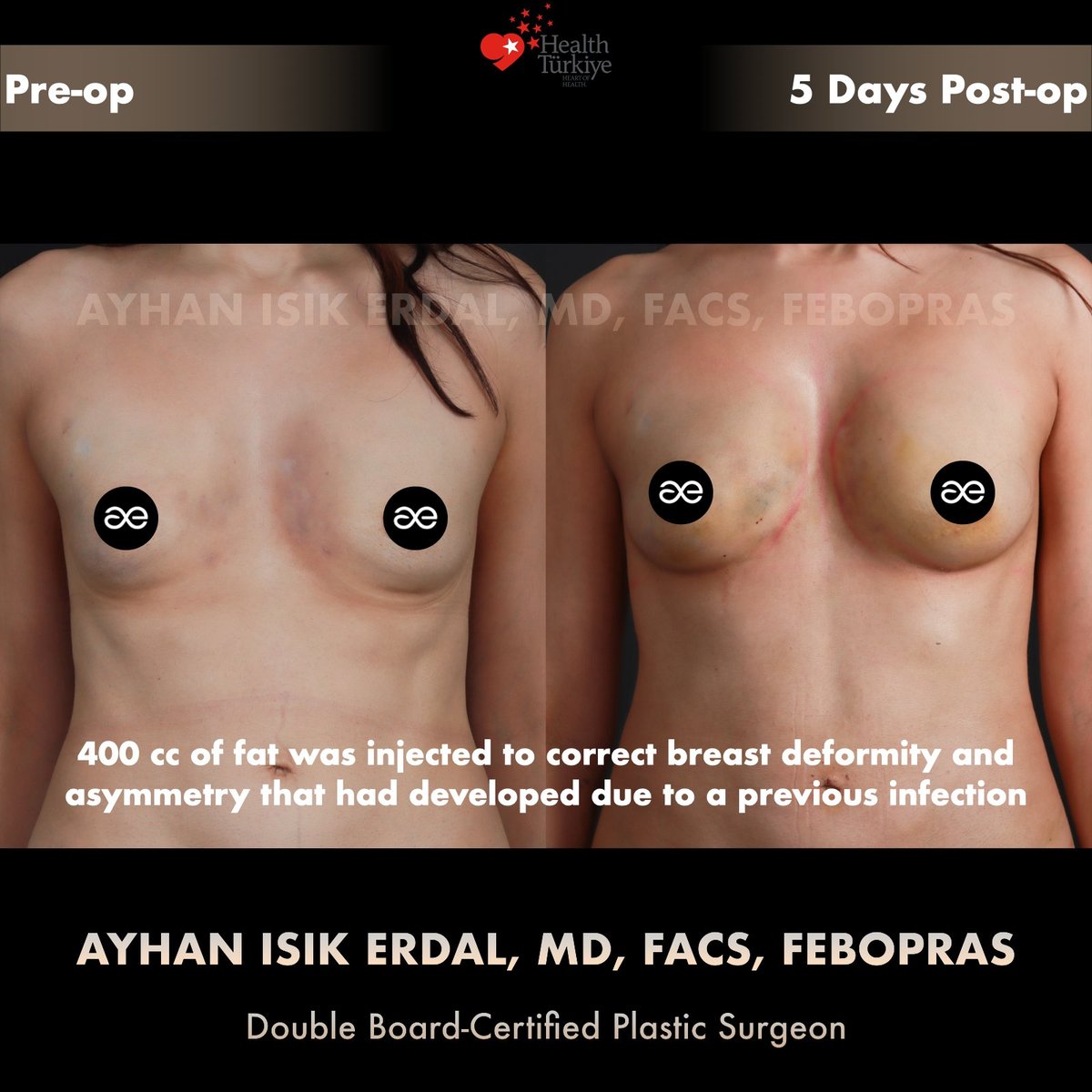
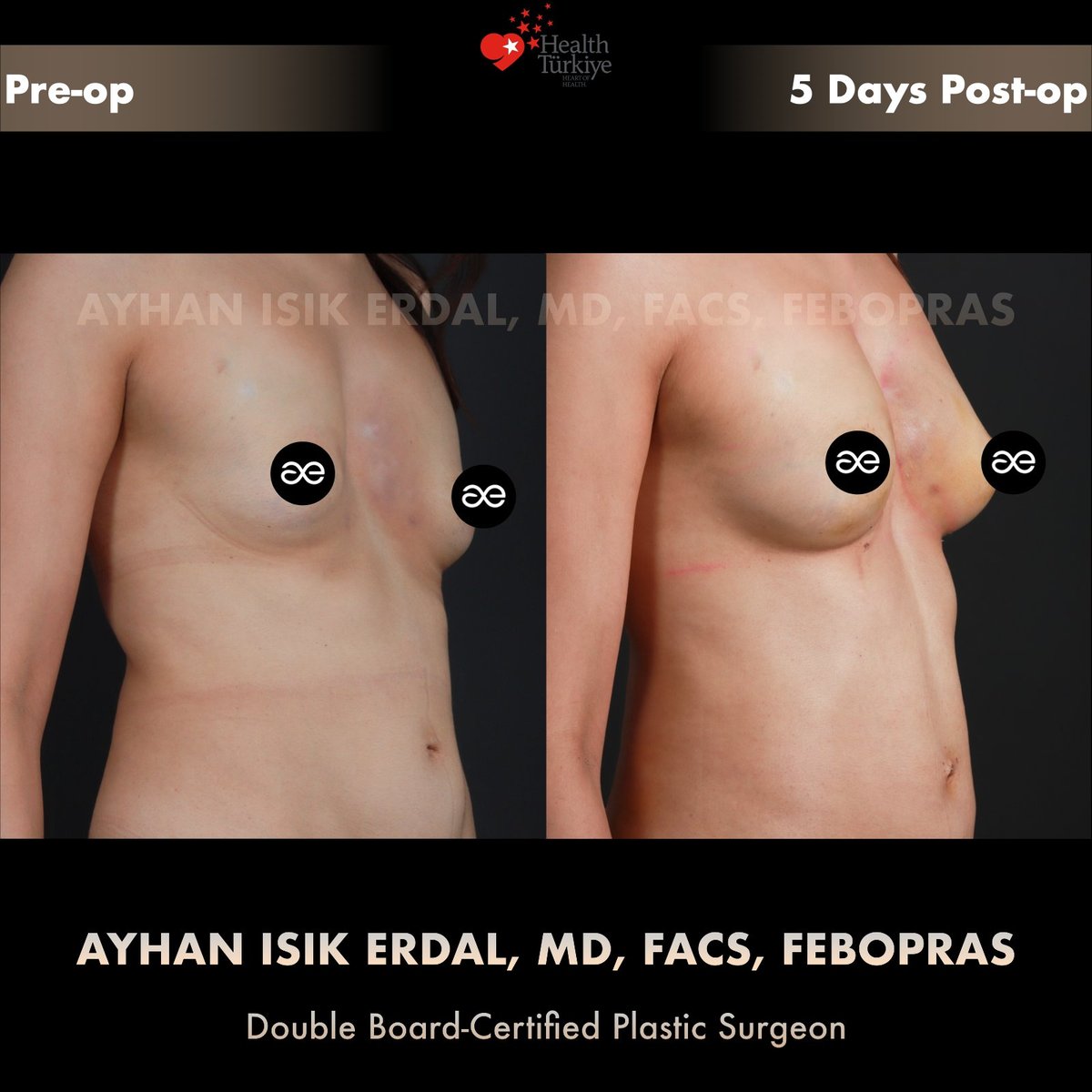
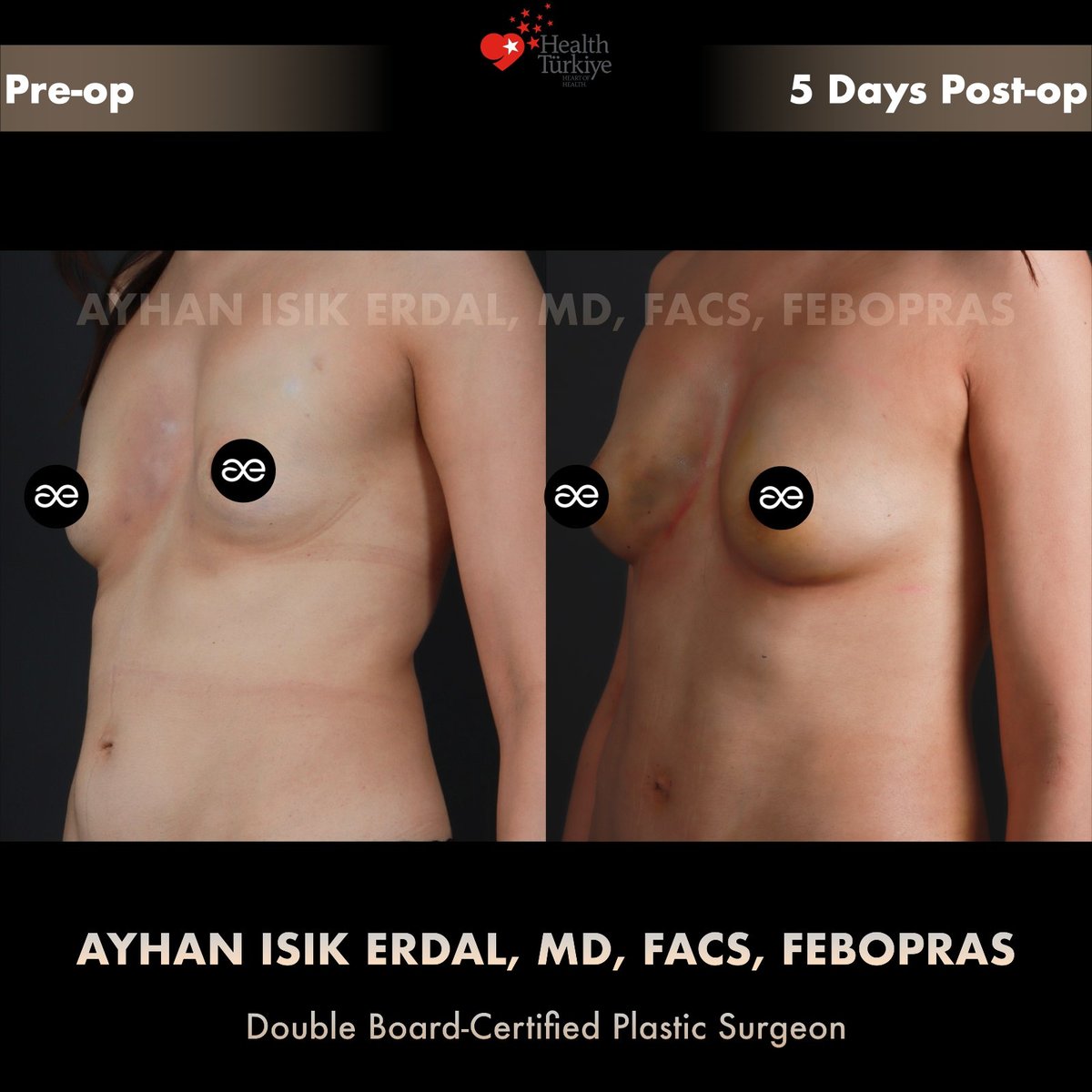
Photos — pre-op and Day 5 post-op
Note on Day 5 photographs. The post-operative images shown below are taken five days after surgery, before discharge from clinic care. Ecchymosis (yellow/green skin discolouration) and post-injection oedema are entirely normal at this stage and resolve over the following 4–8 weeks. The final aesthetic outcome of fat grafting is judged at 6–12 months, after expected resorption has stabilised. We publish Day 5 photos rather than only "best-light" final results because honest documentation of the recovery process is part of how informed patients evaluate a surgeon.
Technique notes
High-volume fat grafting is technically demanding. Three principles drive the technique:
Atraumatic harvest
Fat cells (adipocytes) are fragile. Aggressive cannulation, high-pressure suction, or rapid liposuction damages the cells before they can be re-injected. Harvest is performed at low negative pressure with cannulas chosen to preserve cell architecture.
Proper processing
Lipoaspirate contains fat, blood, oil, and tumescent fluid. Only the viable adipose fraction should be re-injected. Processing — whether by decantation, centrifugation, or filtration — separates the usable fat from the rest. Improperly processed fat produces poor graft survival and increases the risk of fat necrosis.
Layered, low-volume injection
Each individual deposit of fat must be small enough that surrounding tissue can vascularise it within the critical first 48–72 hours. Injecting large bolus volumes guarantees central necrosis. The technique places fat in many small parcels across multiple tissue planes — subcutaneous, subglandular, and (when appropriate) intramuscular — using small cannulas with retrograde injection on withdrawal.
For this case, 400 cc total volume was distributed as hundreds of individual passes, each depositing approximately 1–2 cc per pass.
Early recovery — what you see at Day 5
The Day 5 photographs show what is typical for this stage of recovery from high-volume fat grafting:
- Visible ecchymosis — the yellow/green discolouration is haemoglobin breakdown products from minor bleeding at injection sites. This is universal in fat grafting and resolves over 2–3 weeks.
- Post-injection oedema — soft-tissue swelling makes the breasts look fuller at Day 5 than they will appear at Week 4 or Month 3. Some of the apparent volume seen here is fluid, not fat.
- Donor site discomfort — abdomen and flanks are tender and bruised, requiring compression garment for 4–6 weeks.
- Soft, mouldable consistency — at Day 5 the grafted tissue is still oedematous and not firm. Final consistency develops over 6–12 weeks.
Pain is typically well-controlled with oral analgesics. Most patients return to office work within 7–10 days. No restriction on upper-body movement is required for the breast component; donor site tenderness is the main limiting factor.
Expected trajectory from Day 5 to final outcome
- Week 1 (Day 5 photo): Bruising peak, swelling near peak, breasts appear larger than final result will be.
- Weeks 2–4: Bruising resolves. Swelling decreases significantly. Breast volume appears to "shrink" — this is fluid resorption, not fat loss.
- Months 2–3: The fat that did not establish vascular supply is resorbed by the body. Typical resorption rate is 30–40%, meaning approximately 60–70% of the injected volume becomes permanent. Volume continues to settle.
- Months 4–6: Final volume becomes apparent. The grafted fat is now permanent and behaves like the patient's own tissue — gaining or losing volume with weight changes, moving naturally.
- Months 6–12: Final aesthetic outcome. Skin softens further. Any small areas of fat necrosis (uncommon in well-executed cases) become apparent if present.
- Touch-up consideration: If additional volume is desired, a second fat-grafting session is straightforward at 6–12 months. The initial graft has stabilised by then and the new injection adds onto a vascularised base.
What this case demonstrates
- Revision after failed primary surgery does not always require implants. In carefully selected patients, fat grafting alone produces an acceptable correction without the complications of prosthetic placement in compromised tissue.
- High-volume single-session fat grafting (400 cc total) is achievable when harvest, processing, and injection technique are executed properly.
- Day 5 photographs honestly show what early recovery looks like — bruised, swollen, but with the underlying correction visible. Patients who expect "Instagram-final" appearance immediately after fat grafting will be disappointed; patients prepared for the actual recovery trajectory typically are not.
- Patient preference matters in revision planning. A patient who has had infection in implant-related tissue and prefers to avoid further prosthetic exposure has a clinically reasonable position. Respecting that preference and offering a non-implant solution is good revision practice — not a compromise.
Considering revision without implants?
If your previous breast surgery did not go well and you would prefer a non-implant solution, send your photos and history. We will tell you honestly whether fat grafting is appropriate for your case.
Free WhatsApp Consultation